Barrett's Esophagus
OVERVIEW | CAUSES | RISK FACTORS | SYMPTOMS | COMPLICATION | Diagnosis | TREATMENT | REFERENCES
Overview
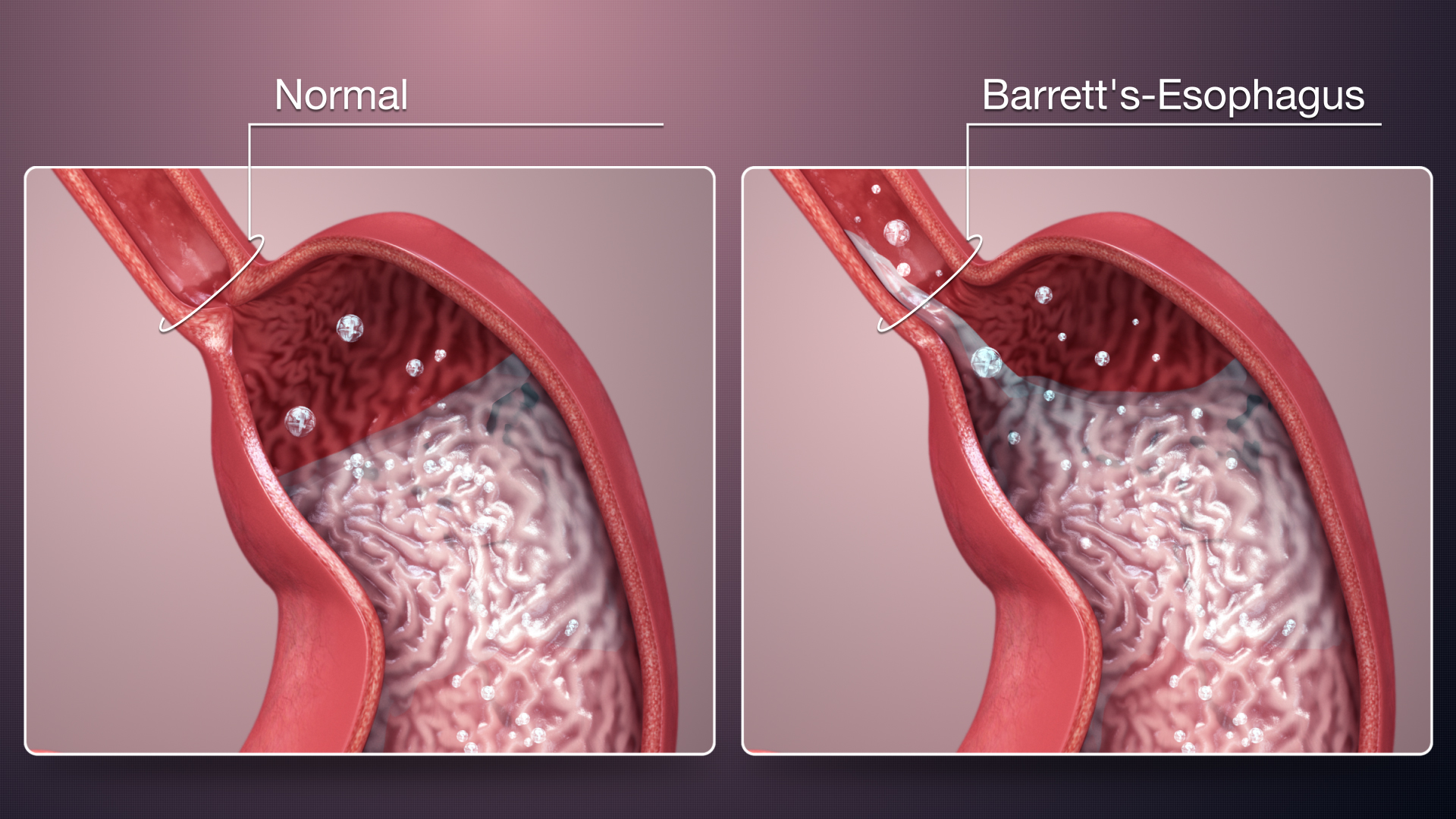
Barrett’s esophagus is a condition in which the cells that make up your esophagus begin to look like the cells that make up your intestines. This often happens when cells are damaged by exposure to acid from the stomach.
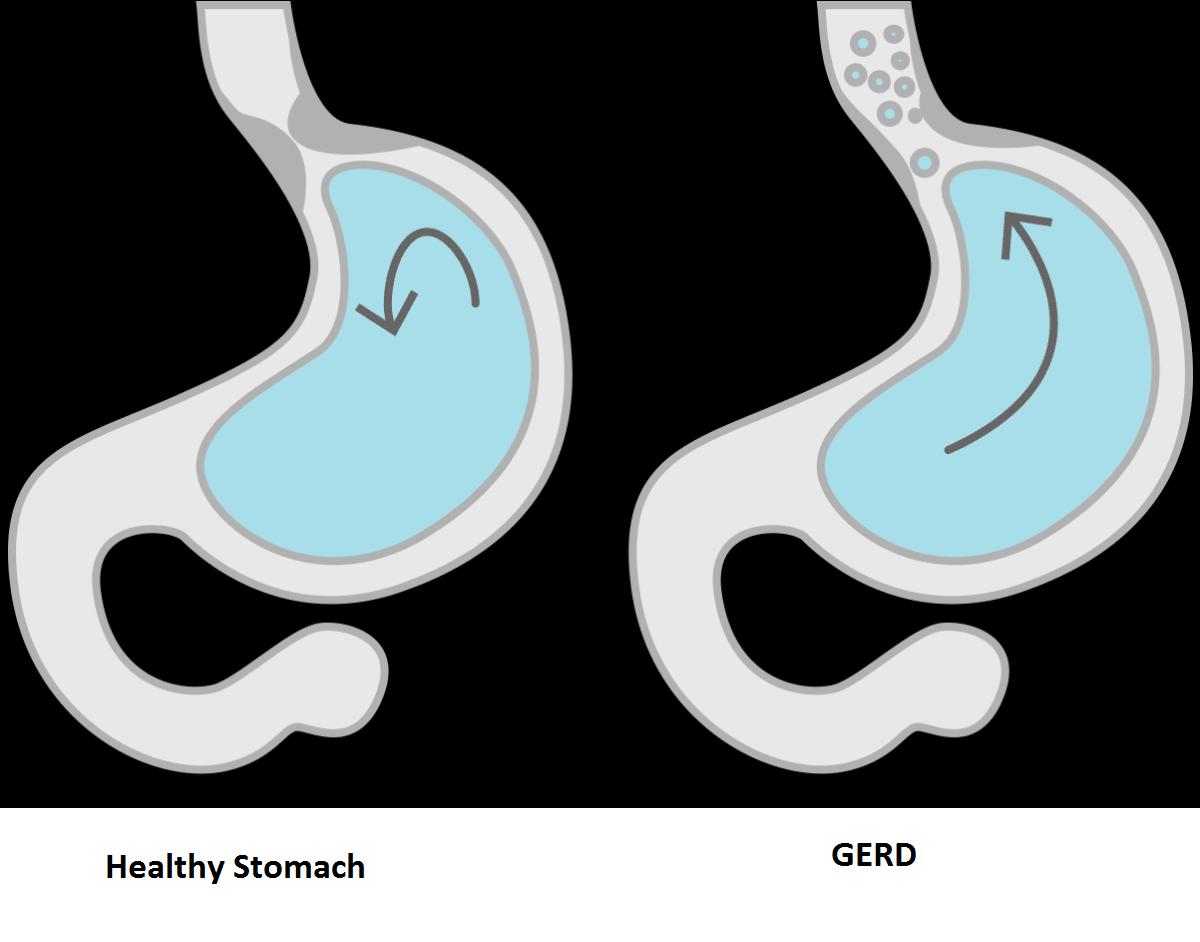
This condition often develops after years of experiencing gastroesophageal reflux (GERD). In some cases, Barrett’s esophagus can develop into Esophageal Cancer.
Causes
The exact cause of Barrett's esophagus isn't known. While many people with Barrett's esophagus have long-standing GERD, many have no reflux symptoms, a condition often called "silent reflux."
Whether this acid reflux is accompanied by GERD symptoms or not, stomach acid and chemicals wash back into the esophagus, damaging esophagus tissue and triggering changes to the lining of the swallowing tube, causing Barrett's esophagus.
Risk factors
Factors that increase your risk of Barrett's esophagus include:
- Family history. Your odds of having Barrett's esophagus increase if you have a family history of Barrett's esophagus or esophageal cancer.
- Being male. Men are far more likely to develop Barrett's esophagus.
- Being white. White people have a greater risk of the disease than do people of other races.
- Age. Barrett's esophagus can occur at any age but is more common in adults over 50.
- Chronic heartburn and acid reflux. Having GERD that doesn't get better when taking medications known as proton pump inhibitors or having GERD that requires regular medication can increase the risk of Barrett's esophagus.
- Current or past smoking.
- Being overweight. Body fat around your abdomen further increases your risk.
Symptoms
Barrett’s esophagus does not have any symptoms. However, because most people with this condition also have GERD, they will usually experience frequent heartburn.
Call your doctor right away if any of the following symptoms occur:
- Chest pain
- Vomiting blood, or vomit that resembles coffee grounds
- Difficulty in food or liquid swallowing
- Passing black, tarry, or bloody stools
Complications
People with Barrett's esophagus have an increased risk of esophageal cancer.
Diagnosis
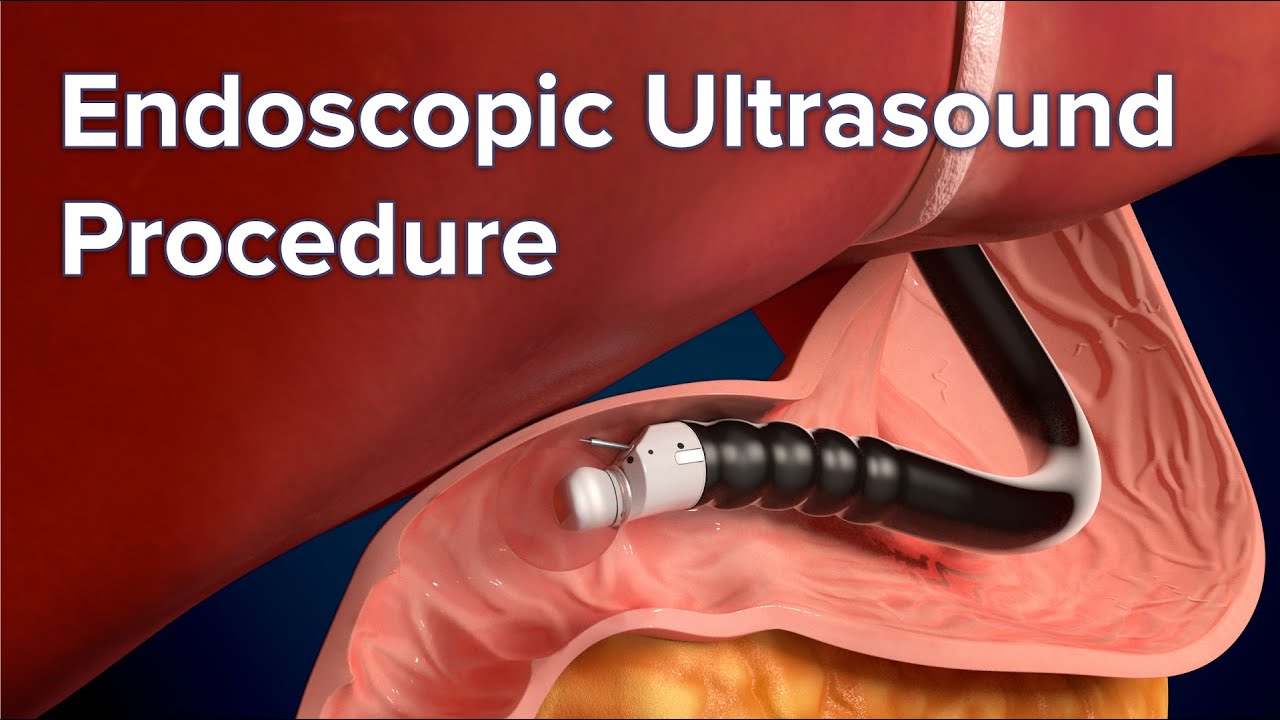
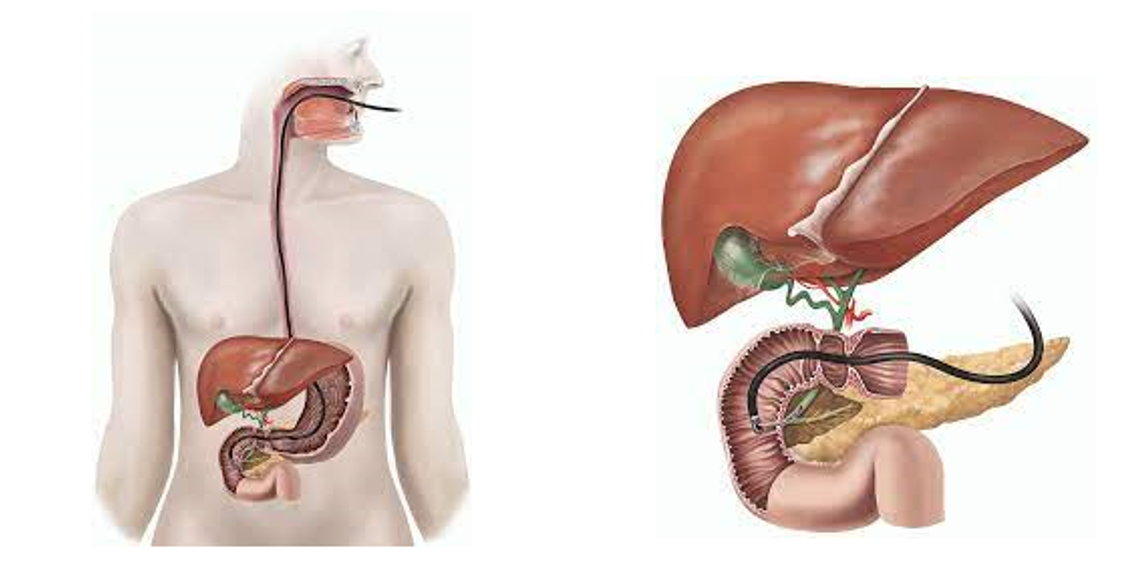
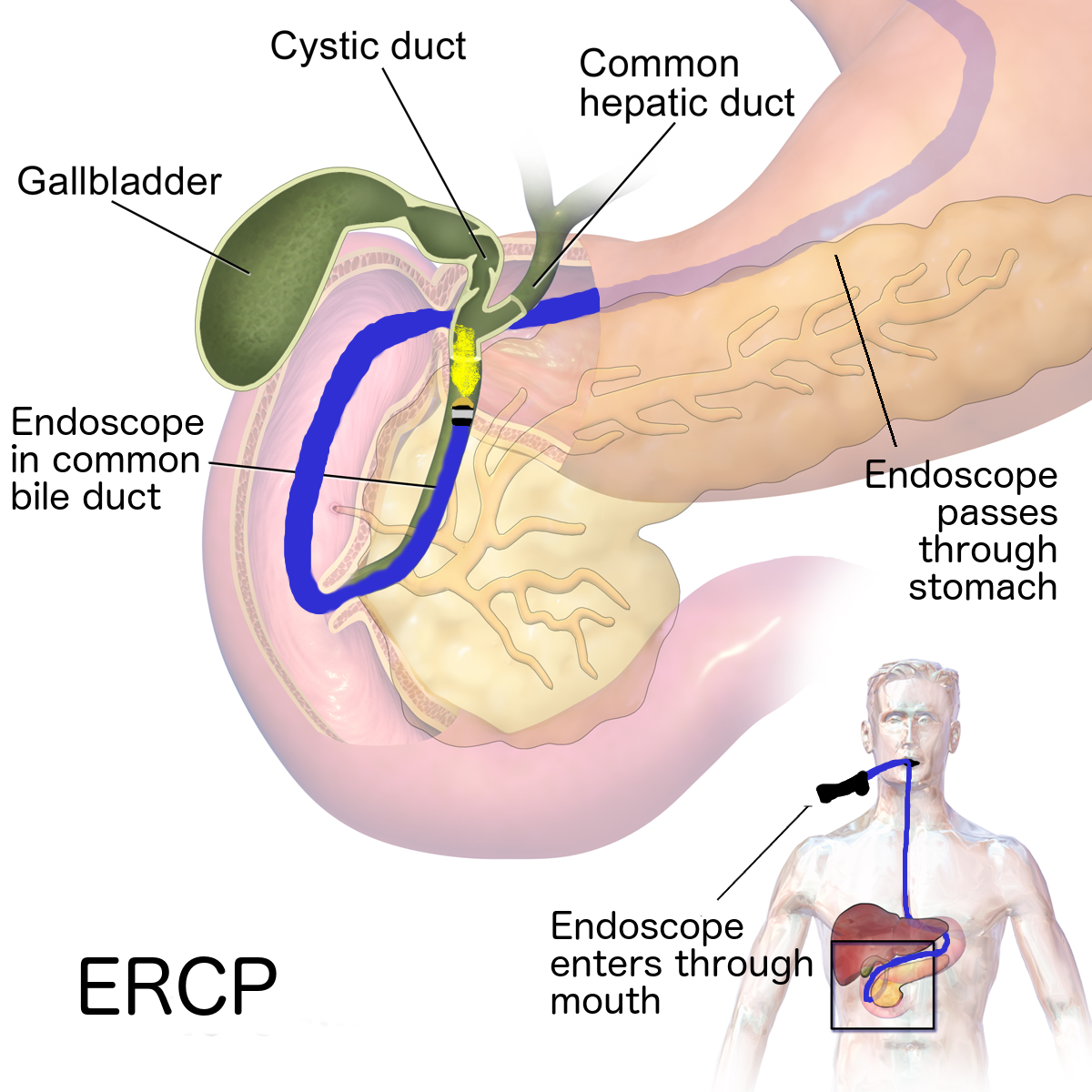
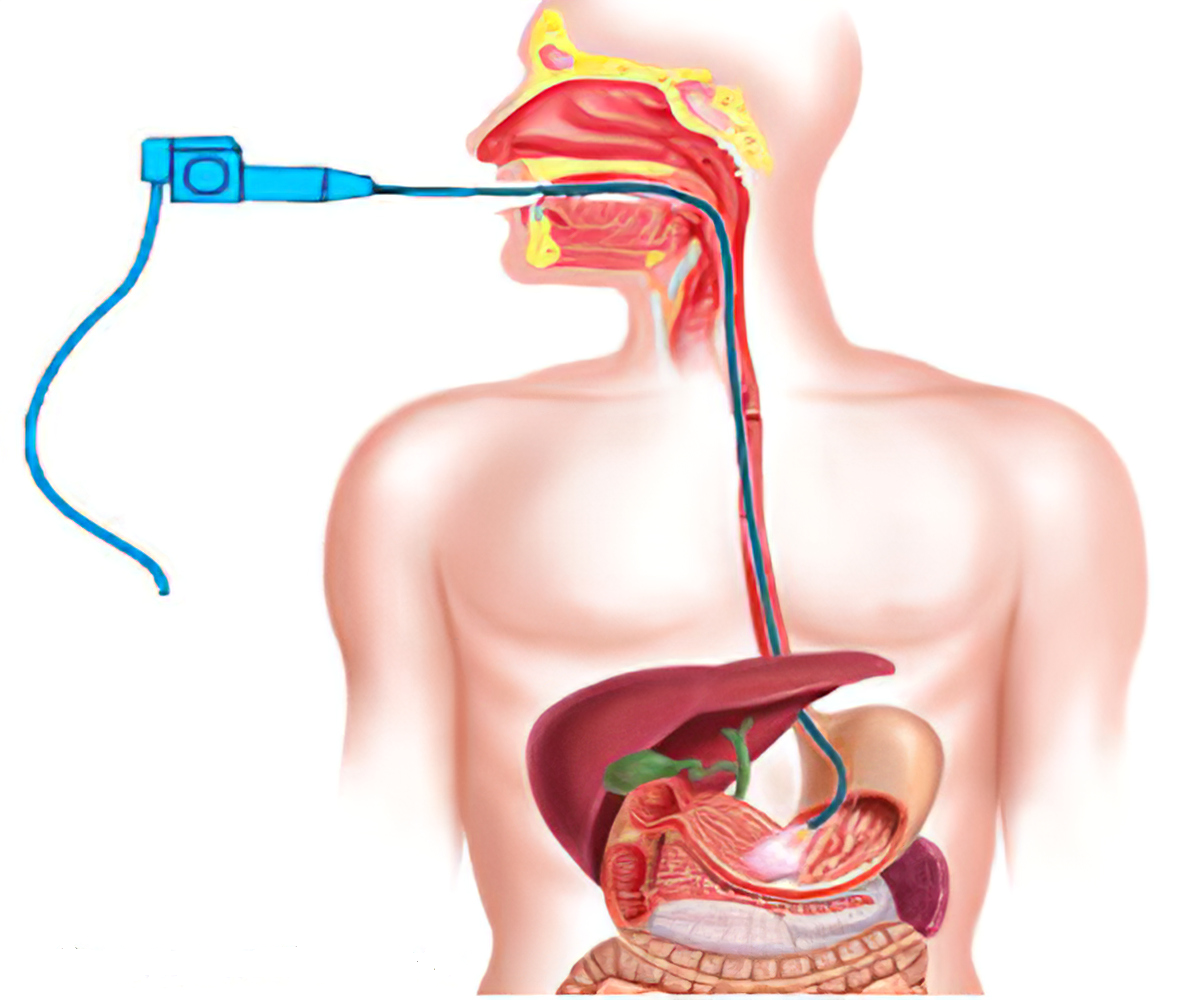
If your doctor suspects that you have Barrett’s esophagus they may order an endoscopy. An endoscopy is a procedure that uses an endoscope, or a tube with a small camera and light on it. An endoscope allows your doctor to see the inside of your esophagus.
Your doctor will be checking to make sure that your esophagus looks pink and shiny. People who have Barrett’s esophagus often have an esophagus that looks red and velvety.
Your doctor may also take a tissue sample that will allow them to understand what changes are going on in your esophagus. Your doctor will examine the tissue sample for dysplasia, or the development of abnormal cells.
The tissue sample be ranked based on the following degrees of change:
- No dysplasia: no visible cell abnormalities
- Low grade dysplasia: small amount of cell abnormalities
- High grade dysplasia: large amount of cell abnormalities and cells that may become cancerous.
Treatment
Treatment for Barrett’s esophagus depends on what level of dysplasia your doctor determines you have.
Options may include:
1. No or low-grade dysplasia
If you have no or low-grade dysplasia, your doctor will likely recommend treatments that will help you manage your GERD symptoms. Medications to treat GERD include H2-receptor antagonists and proton pump inhibitors.
You may also be a candidate for surgeries that can help you manage your GERD symptoms. There are two surgeries that are commonly performed on people with GERD, which include:
i. Nissen Fundoplication:
This surgery attempts to strengthen the lower esophageal sphincter (LES) by wrapping the top of your stomach around the outside of the LES.
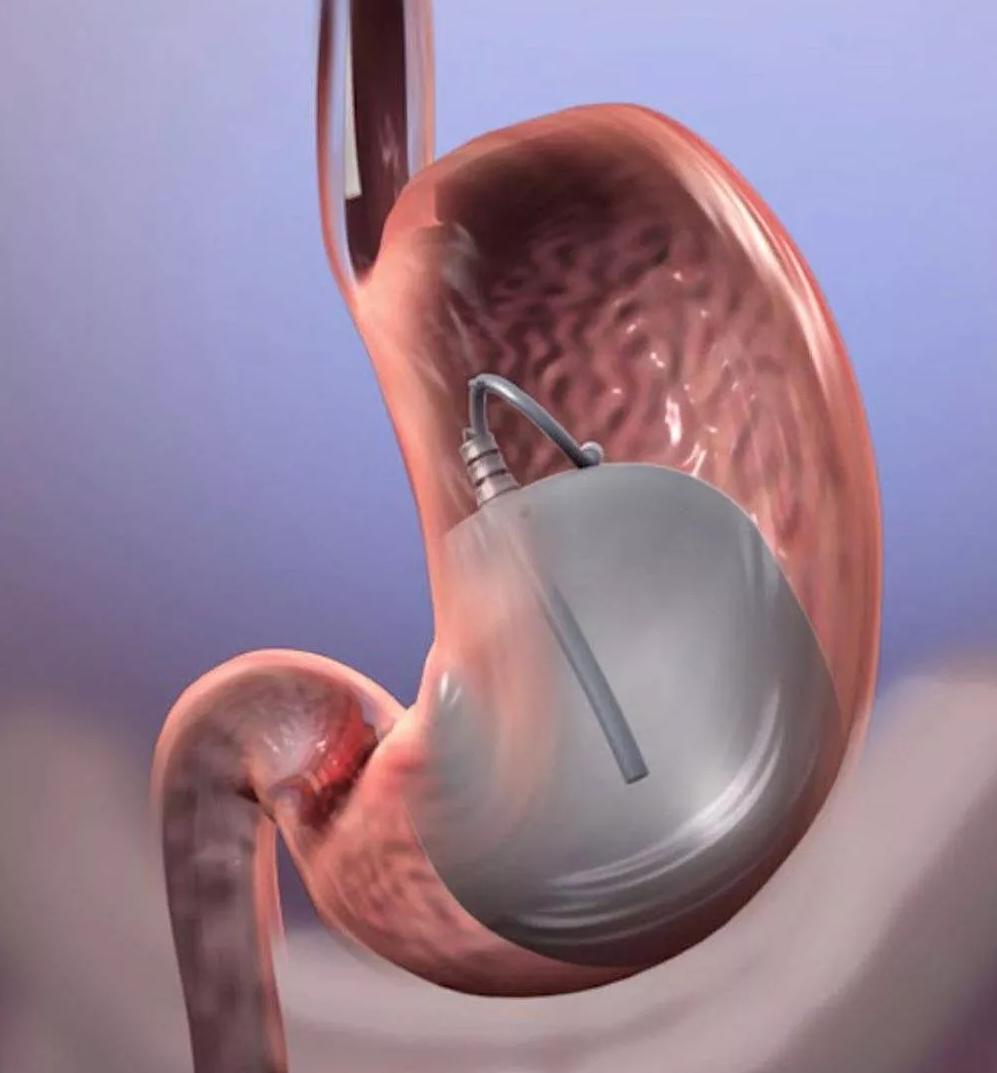
ii. LINX:
In this procedure, your doctor will insert the LINX device around lower esophagus. The LINX device is made up of tiny metal beads that use magnetic attraction to keep the contents of your stomach from leaking into your esophagus.
iii. Stretta procedure:
A doctor performs the Stretta procedure with an endoscope. Radio waves are used to cause changes in the muscles of the esophagus near where it joins the stomach. The technique strengthens the muscles and decreases reflux of the stomach contents.
2. High grade dysplasia
Your doctor may recommend more invasive procedures if you have high-grade dysplasia. For example, removing damaged areas of the esophagus through the use of endoscopy. In some cases, entire portions of the esophagus are removed. Other treatments include:
i. Radiofrequency ablation
This procedure uses an endoscope with a special attachment that emits heat. The heat kills abnormal cells.
ii. Cryotherapy
In this procedure, an endoscope dispenses cold gas or liquid that freeze the abnormal cells. The cells are allowed to thaw, and then are frozen again. This process is repeated until the cells die.
iii. Photodynamic therapy
Your doctor will inject you with a light-sensitive chemical called porfimer (Photofrin). An endoscopy will be scheduled 24 to 72 hours after the injection. During the endoscopy, a laser will activate the chemical and kill the abnormal cells.